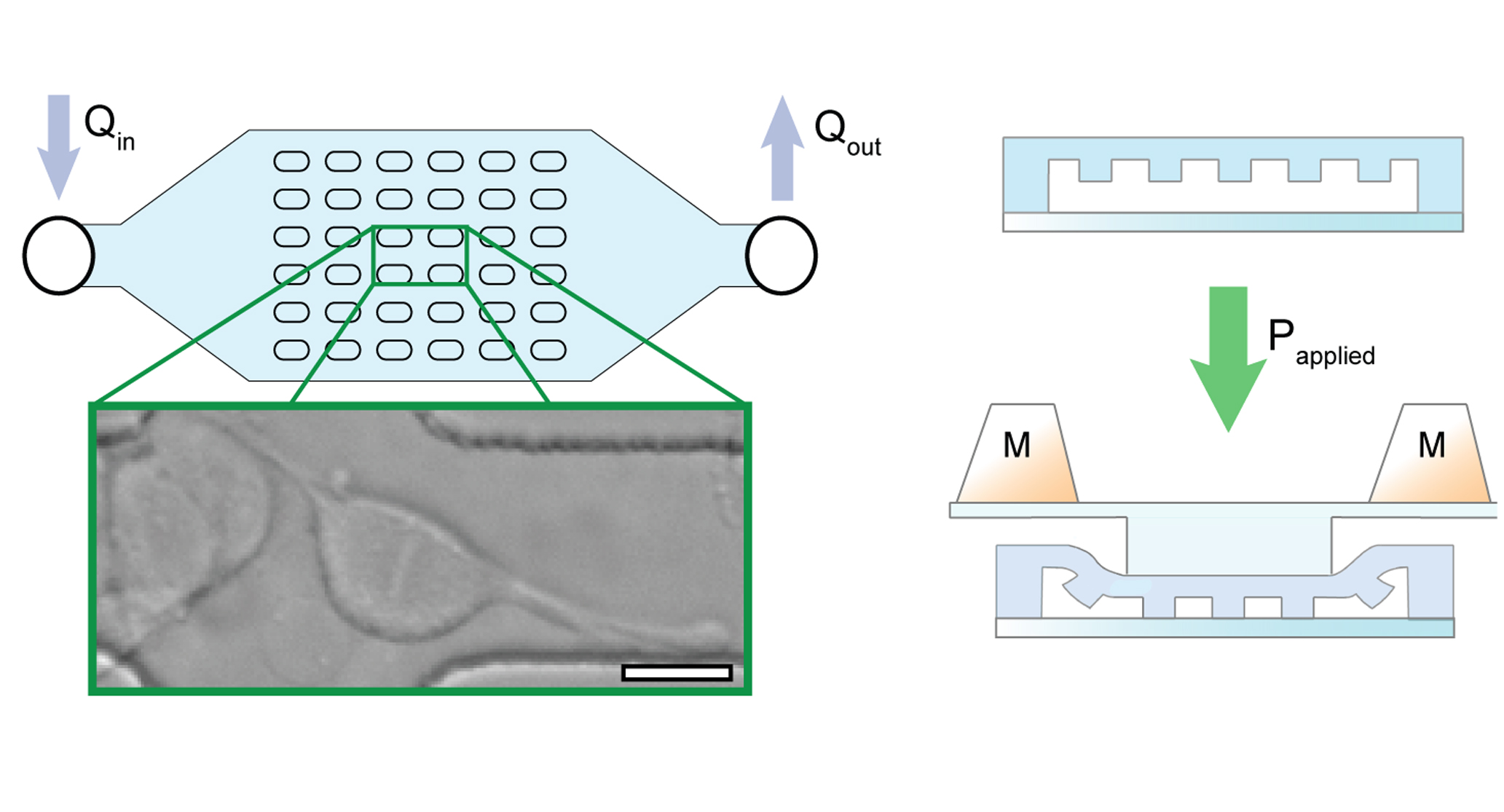
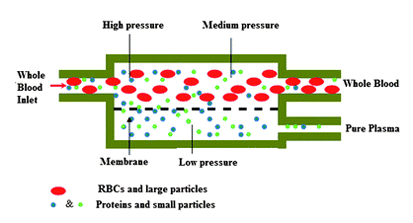
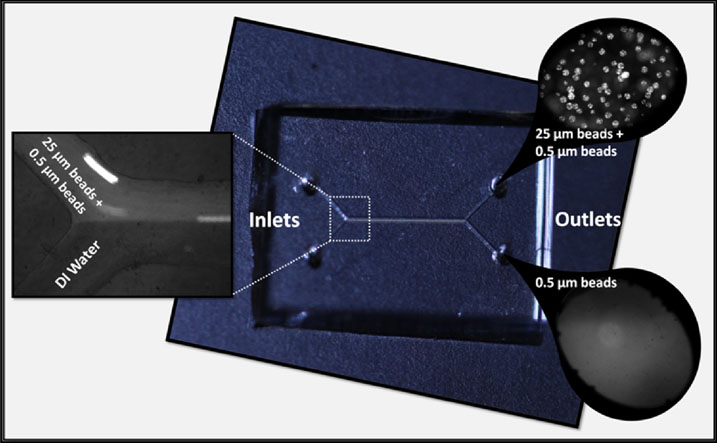
Continuously Sorting Particles According to Shape
Academic Research
Dino Di Carlo
Lab on a Chip
RSC Lab on a Chip
UCLA
There are numerous filters to separate particles in liquid based on their size, which can be enough to isolate them; however, particle shape can be more important, as it…
Tracking Immune Responses to Food with a Gut on a Chip
Academic Research
RSC Lab on a Chip
Immunology
Lab on a Chip
Ecole Polytechnique Federale de Lausanne
In an effort to model the complex processes occurring in human bodies, Donald Ingber has pioneered the development of ‘organs-on-chips,’ reproducing the lung and the gut on microfluidic devices. These systems allow researchers to replicate and study organs without the use of human test subjects. While this…
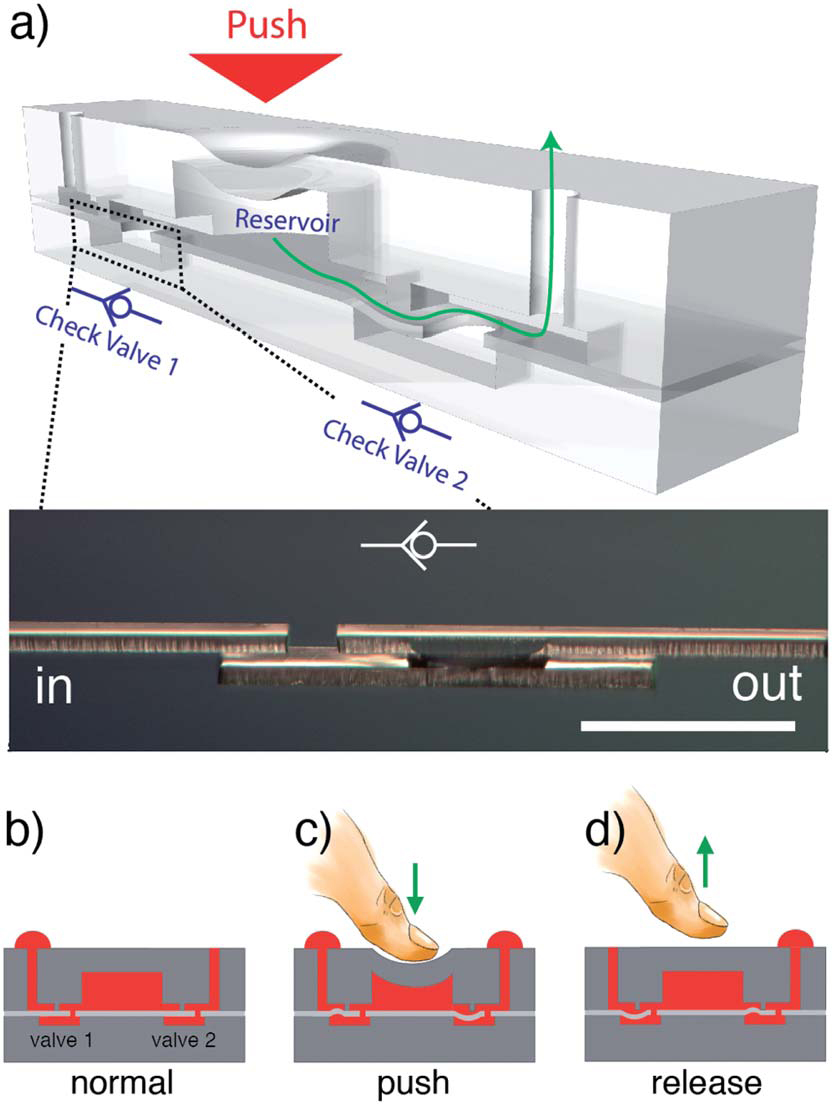
A Microsyringe to Take the Pain out of Shots
Academic Research
Lab on a Chip
Hematology
RSC Lab on a Chip
Back when I was in sixth grade, I remember reading a little blurb in some science magazine at school that in the future we could receive shots via a method that would feel…
Studying the Effects of Confinement on Cell Division
Academic Research
Oncology
Lab on a Chip
UCLA
Dino Di Carlo
PLoS ONE
On Microfluidic Future I like reviewing advancements in therapeutic or diagnostic…
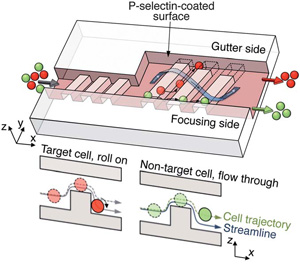
Rolling Out Cell Sorting with Microfluidics
Academic Research
RSC Lab on a Chip
Lab on a Chip
Rohit Karnik
MIT
Cells are quite valuable, especially when used for regenerative research, diagnostics or research. But harvested cells do not come presorted and need to be separated from a…
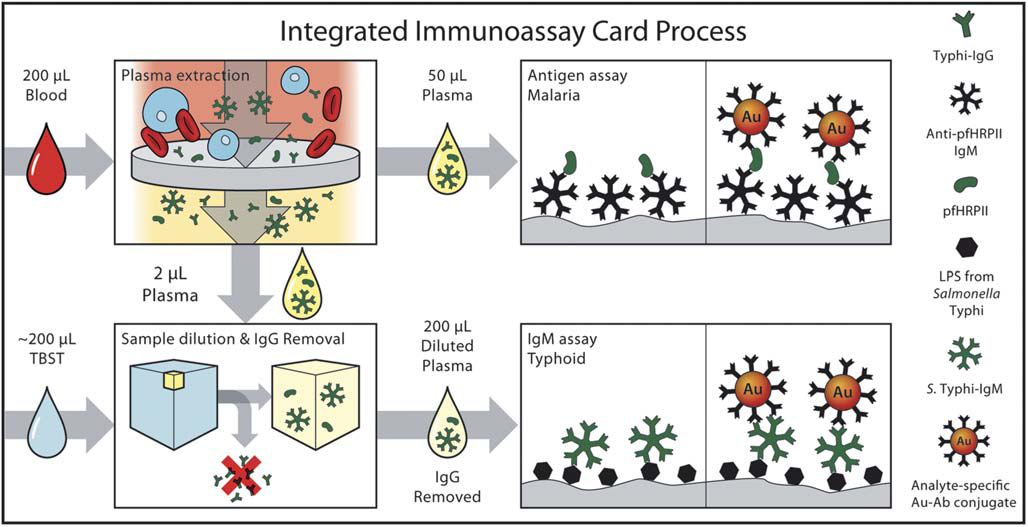
Diagnosing Similar Diseases in Low Resource Settings
Academic Research
Diagnostics
Hematology
Point of Care
RSC Lab on a Chip
Immunoassay
Paul Yager
Lab on a Chip
A lot of excitement surrounding microfluidics has been about its promising use in diagnosis in low-resource settings. Many infectious diseases present in developing…
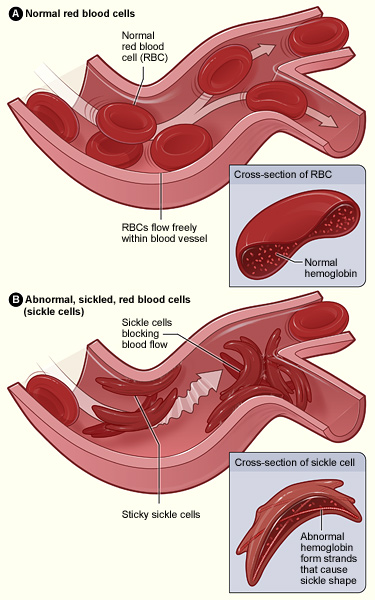
Narrowing the Gap to Characterize Sickle Cell Disease
Academic Research
Lab on a Chip
Hematology
MIT
Harvard
Diagnostics
Microfluidic Future is by no means an accurate representation of all the current, ongoing research in microfluidics. Nevertheless, the fact that you won’t be able to find…
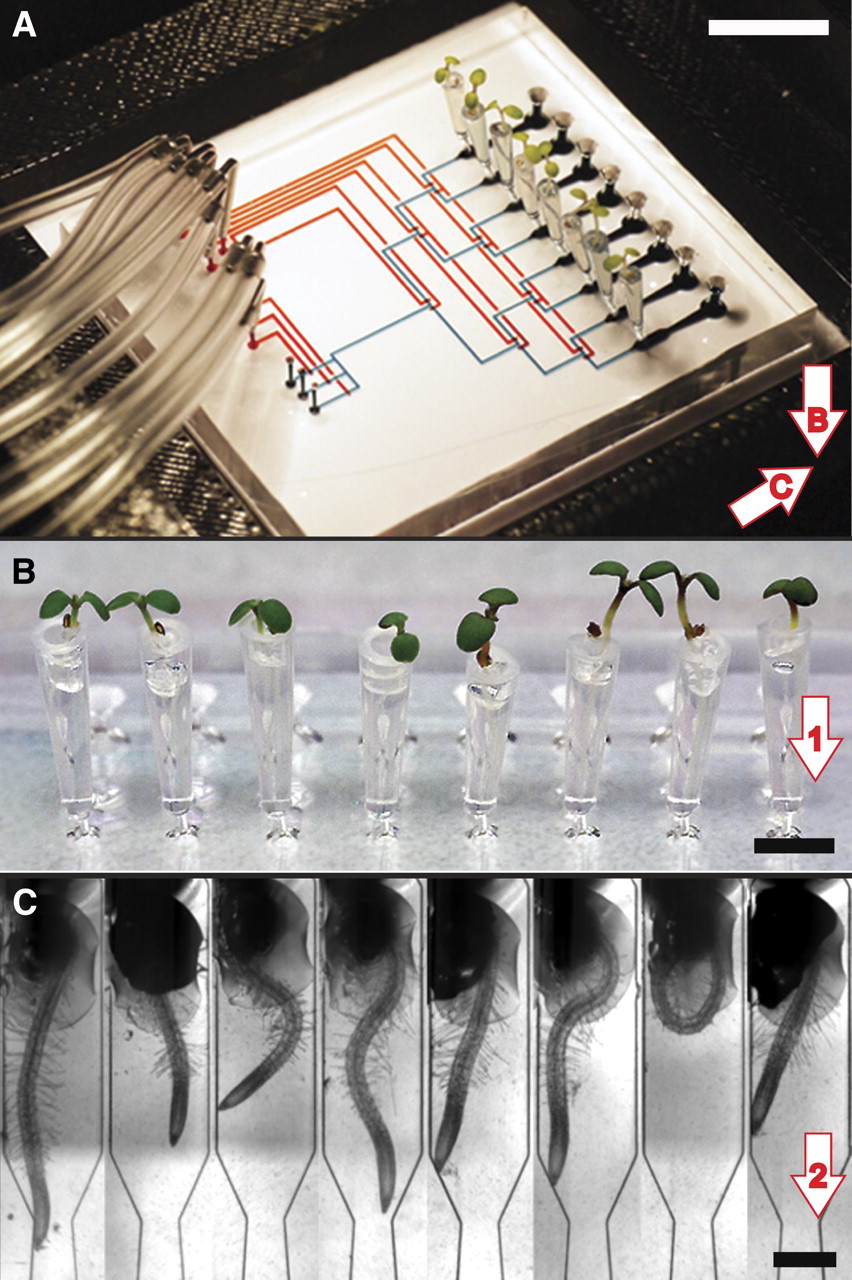
Getting to the Root of Microfluidics
Academic Research
Lab on a Chip
Stephen Quake
Stanford University
It’s not hard to see that a lot here at Microfluidic Future focuses on the medical applications of microfluidics, but that doesn’t mean that I’m not interested in other ways…
A Case for Oral Diagnostics with Microfluidics
Academic Research
Rice University
John T McDevitt
Point of Care
Oral Fluids
Periodontal Disease
Pharmacogenomics
Well, a lot of things, but let’s start with the basics. In order to use a microfluidic device, you need some type of fluid right? Sure if you had some powder or fine…
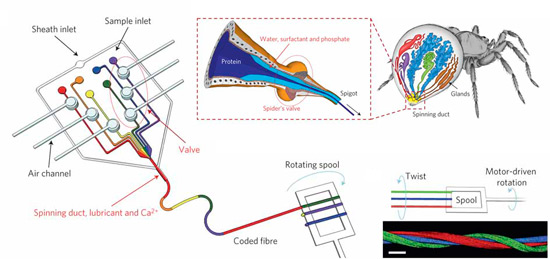
Spin Silk Like a Spider! No Legs Required (Just Microfluidics)
Academic Research
Tissue Engineering
Nature
Biomimetics
Author’s note: This post was chosen as an Editor’s Selection at ResearchBlogging.org. Thanks for the support!
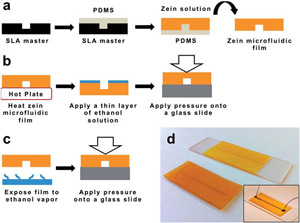
You Eat Corn? I Make Microfluidics with It
Academic Research
Materials
Lab on a Chip
RSC Lab on a Chip
Some of us are on the search for new renewable materials that can make our lifestyle a bit more sustainable. Although a new resource may be renewable, that doesn’t mean it…
Microfluidics… In Space?
Industry News
Point of Care
Lab on a Chip
Popular Science
Diagnostics
Radisens Diagnostics
What realm of life is safe from microfluidics? Hopefully none, as the technology continues to work its…
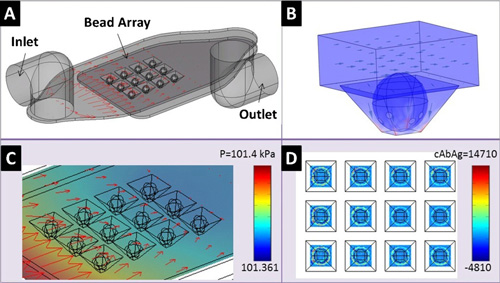
Bloodhound Beads Sniffing out Heart Attacks
Academic Research
Diagnostics
Immunoassay
Rice University
John T McDevitt
Point of Care
Hematology
Oral Fluids
How would you detect a heart attack? There are some symptoms that might tell you that you are very likely having a heart attack. Although you might feel pain in the chest…
PDMS: The Favorite Material of Microfluidics (for now)
Academic Research
Microfluidics Basics
Materials
Harvard
George M Whitesides
Whether you’ve been learning about microfluidics here at Microfluidic Future or somewhere…
Detecting Ovarian Cancer with a Cell Phone and a Microfluidic Chip
Academic Research
Cell Phone
Utkan Demirci
Immunoassay
ELISA
Diagnostics
Harvard
Point of Care
RSC Lab on a Chip
Urinalysis
Oncology
Author’s note: This post was chosen as an Editor’s Selection at ResearchBlogging.org. Thanks for the support!
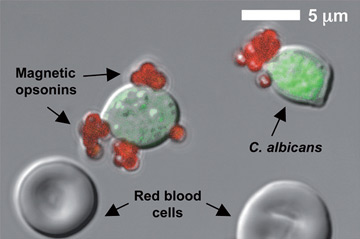
Clearing Sepsis with Magnetic Microfluidics
Academic Research
Wyss Institute
Harvard
Donald Ingber
Lab on a Chip
Point of Care
Therapeutics
RSC Lab on a Chip
Hematology
Seps…
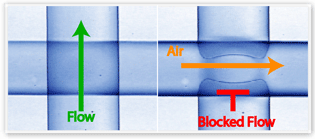
The Microvalve: The Traffic Light of Microfluidics
Academic Research
Lab on a Chip
Microvalves
Stephen Quake
Harvard
George M Whitesides
RSC Lab on a Chip
Microfluidics Basics
You could say that valves in microfluidics (or microvalves) are like traffic lights that control flow along microfluidic channels. But I’d say that they’re more like police…
SIMBAS, Everything the Blood Touches Is Our Kingdom
Academic Research
Immunoassay
Hematology
Daniel Fletcher
Luke Lee
Diagnostics
UC Berkeley
Lab on a Chip
Point of Care
RSC Lab on a Chip
Hey, how’s your biotin? What? No it’s not an organic metal, maybe you call it B7? You’re probably fine, but have you been depressed, lethargic or losing your hair lately?…
Microfluidics? What’s That? A Beginner’s Guide
Academic Research
Microfluidics Basics
Stephen Quake
Paul Yager
Nature
Lab on a Chip
George M Whitesides
Albert Folch
Education
Point of Care
Harvard
Author’s note: This post was chosen as an Editor’s Selection at ResearchBlogging.org. Thanks for the support!
Filtering Blood During Cardiopulmonary Bypass (CPB)
Academic Research
Hematology
Rutgers University
Jeffrey Zahn
Filtration
Cardiopulmonary Bypass
Anticoagulant
RSC Lab on a Chip
More than 1,000 adult and 50 pediatric patients undergo a surgery involving cardiopulmonary bypass (CPB) each day in the United States. A CPB is used when performing surgery…
Building Cartilage Scaffolds the Microfluidic Way
Academic Research
Biomaterials
Cartilage
Digital Microfluidics
National Taiwan University
Scaffold
Our bodies are pretty much amazing. We can get hurt, and our bodies will heal our cuts and bones (with the right support). But not everything heals so easily, like…
Decoding Liquids Before Your Very Eyes
Academic Research
Diagnostics
Wettability
Harvard
Joanna Aizenberg
Journal of the American Chemical Society
Point of Care
Wyss Institute
Seeing really is believing. How often can we tell what a liquid is by just looking at it? Not too often. Sure, you might be able to tell when you definitely smell something sulfurous, or have a slippery base and I hope you can pick out milk. But we’re not always that lucky, especially if you’re dealing with something you really…
Vortices, not Vortexing: Replacing the Centrifuge with a Lab-on-a-Chip
Academic Research
Hematology
RSC Lab on a Chip
Lab on a Chip
UCLA
Dino Di Carlo
In case you didn’t get the first part of my title, let me tell you a little about centrifugation. Centrifugation is a very common research technique. A solution is…
Mendeley: Scientific Article Organizer for PDFs
Research Tools
Organization
Scientific Article
Mendeley
For the past 6 months or so I’ve been using Mendeley to organize my PDFs. It’s a program that allows you to organize and maintain your scientific articles. While you might be able to implement your own nomenclature and folder…
Microfluidics Education
Academic Research
AIP Biomicrofluidics
UC Irvine
Thermoplastics
Michelle Khine
Low Cost Microfluidics
Education
The extent to which someone develops their…
Creating Droplets in Microfluidic Devices with Ultraviolet Light
Academic Research
Digital Microfluidics
Damien Baigl
RSC Lab on a Chip
Wettability
École Normale Supérieure
With the widespread use of electronics, we often use the word…
No matching items