Cardiopulmonary Bypass
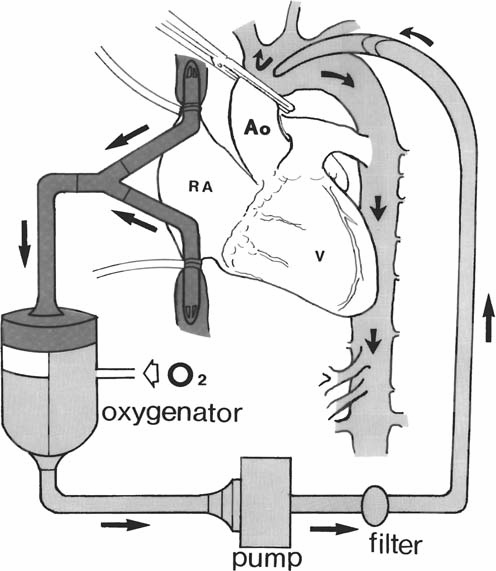
More than 1,000 adult and 50 pediatric patients undergo a surgery involving cardiopulmonary bypass (CPB) each day in the United States. A CPB is used when performing surgery on the heart or lungs, leaving them unable to perform their normal functions. But CPB introduces a lot of foreign material to the body, creating adverse reactions. The CPB assembly, drugs and surgical processes can each have their own inflammatory effects. Induced inflammatory responses may include “complement, neutrophil, and platelet activation, endothelial dysfunction, and the release of proinflammatory cytokines.” Analyzing the patient’s blood during CPB is necessary to tie an inflammatory response to its origin in order to reduce a systemic inflammatory response syndrome (SIRS). But in order to monitor the patient’s status, at least 3 ml of blood must be drawn from the CPB system each time. This blood must then be centrifuged to access its plasma component (read more about a recent centrifuge-on-a-chip). Three ml of blood isn’t needed to get an accurate reading, but it fits into the current operating procedures. This looks like the perfect opportunity to implement a microfluidic device to continuously filter small volumes of plasma from the CPB system to be analyzed, which is exactly what researchers from Rutgers University did.
Microfilter
The article “Microfiltration platform for continuous blood plasma protein extraction from whole blood during cardiac surgery” by Jeffrey Zahn et al. is featured in the 2011 issue 17 of Lab on a Chip. The authors wanted to create a lab-on-a-chip component to filter plasma from CPB while collecting only 50-100 µl every 15 minutes, which could be used for the duration of a procedure which may last 4 hours. The proposed device is simple and features two microfluidic channels separated by a semipermeable membrane. In order to increase the filtration rate, the device features 32 channels in parallel. The authors chose to use a membrane with a 200 nm pore size, which allows plasma and proteins of interest to cross into the filter channel while stopping the 6-8 µm red blood cells (RBC). Even though the pores are sized so that only proteins and plasma can pass, that doesn’t mean that they’ll always be able to do so. Some proteins and cells naturally adhere to foreign objects, creating a clot. We don’t want this to happen to our membrane, which could become mostly or completely clogged. While our pore size allows proteins and plasma to pass through at a faster rate than smaller pores, it is more likely to ensnare a cell that can’t pass through. In order to prevent the membrane from clogging, we can introduce an anticoagulant, such as heparin.
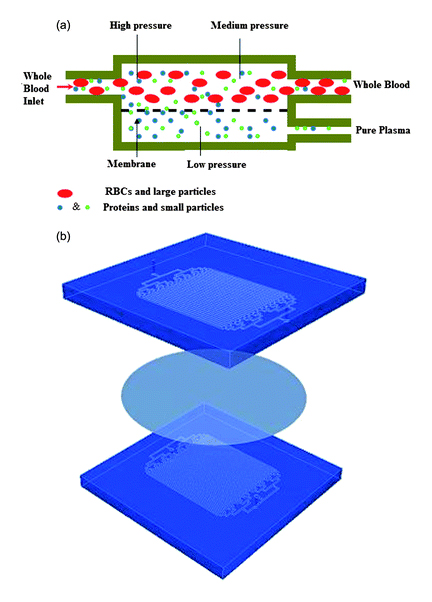
Anticoagulants like heparin prevent blood from clotting by disrupting a series of reactions that occur in blood (To learn more, check out this video on Coagulation Cascade from Johns Hopkins University). We normally don’t want anticoagulants in our blood because it would stop us from healing, but they are used in surgeries to diminish reactions to tools or processes. Instruments can be coated with heparin, which the authors did for the filtration device, so that heparin doesn’t have to be added system-wide. The blood’s hematocrit (Hct) also affects the need for an anticoagulant. Hct represents the percent of the blood volume that is occupied by RBC. The mathematical maximum value would be 1, which would mean that the blood was entirely composed of cells and there was no plasma, while 0 would indicate that there are no cells in the blood. Therefore a higher Hct would have a higher density of cells passing through the device and would need more anticoagulant.
The final device by the authors was able to deliver cell-free plasma which made up 15% of the blood volume. The authors noted that although the plasma is cell-free, they needed to verify the extent of hemolysis. Hemolysis is simply the destruction of RBC. We don’t want this happening to our filtered blood and need to make sure this isn’t the reason that no cells are entering our filtrate.
I think that this is a simple, yet needed piece of equipment. It is basically a membrane separating two microfluidic streams. Although the channels are small (the largest width is no greater than 600 µm), the channels across the membrane are different sizes so that they will still align when put together by our imperfect hands. The construction of parts of the device must be precise, but the device becomes more accessible if it does not need a robot to assemble it. This still needs another attachable point-of-care device to actually test the plasma, but this is promising.
References

Aran, K., Fok, A., Sasso, L., Kamdar, N., Guan, Y., Sun, Q., Ündar, A., & Zahn, J. (2011). Microfiltration platform for continuous blood plasma protein extraction from whole blood during cardiac surgery Lab on a Chip, 11 (17) DOI: 10.1039/C1LC20080A